Rendezvous - when surgical robots meet
- Steve Bell

- Sep 2, 2024
- 13 min read
Updated: Jul 30, 2025

Some background
I’m going to hypothesis something here. Endolumenal robots will have their own right, own place and own capabilities. But an incredible new style of surgery will be unlocked once the endolumenal robots start to meet up with the laparoscopic robots. Rendezvous.
Back in 2007 I was highly involved in creating a company called MINOS Medical (Minimally invasive natural orifice surgery) - and as I like to believe it was way ahead of it’s time.
We were involved in NOTES (Natural Orifice Translumenal Endoscopy Surgery) - where you went into the mouth - or anus or vagina (or uterus in one of our devices) and then passed out across the wall and entered the abdominal space.
It was often called “No Scar” surgery.

But at the same time we also developed a set of tools for NOS (Natural Orifice Surgery) - which was carrying out pretty complex endolumenal therapeutic procedures. So not crossing the wall of the bowel to oesophagus or stomach - but instead staying inside the lumen and operating with pretty advanced instruments inside the structure.
At the time we did some very adventurous work on removing the appendix from inside the lumen through inversion (Appendoectomy) as we termed it. We also did work on inversion and banding closure of diverticulum in the bowel (Diverlite) - thus avoiding later diverticulosis because we closed off the diverticulum (small bowel hernias along the Tenia).
The issue at the time was that endolumenal robots that operated inside structures were just being imagined - and instead we did all of our work using good old fashioned mechanical systems - with a lot of push n pull - a lot of Nitnol flex shape graspers, long overtubes and host of cool stuff.
We also relied heavily on standard endoscopes which made the manoeuvres quite hard. It was especially challenging in the duodenal structures where we were navigating Spyglass scopes through duodenoscopes to look at approaching the gallbladder from an internal chemical ablation approach.
At that time there was some early work going on with companies like Olympus that were working on flexible endoscopic systems and early robots - such as a project known as Endo Samurai.
And there were nascent thoughts from the UK like “Endo Snake” coming from Imperial College.
All pretty much doomed for various reasons - especially as many were focused on NOTES rather than NOS. And it was all a bit confused.

Problems were around reimbursement… who would do it? (The endoscopist or the surgeon)… You needed multi specialty teams of endoscopists and surgeons (way too complex and expensive) to do things that we’re being done very adequately by laparoscopic surgery (and growing laparoscopic robots like daVinci.)
No one could understand why on earth you wanted to take a gallbladder out via traversing the stomach. They were right. People were going after the poster child of laparoscopy — it was a bit dumb.
It was often seen as talking something good that worked - and making it super complex and expensive for no good clinical reason.
Some of the techniques have made it more mainstream such as vNOTES (vaginal NOTES) - and a few very small niche procedures. But NOTES was pretty much doomed back then.
Misunderstanding a GoGo
Back in 2007 / 2008 a few things conspired to make this entire venture an issue. Let’s set aside the biggest issue - which was that there was a banking collapse and housing market collapse that destroyed most VC funding for a few years. So a lot of nascent companies went bankrupt.
The second issue was that the attempt to go transulmenal with a flexible system was just flawed. Mechanical systems were not stable enough or able yo have the fine dextrous control, robotic systems were way too early.
The other massive misunderstanding was the value of NOS rather than NOTES. People could not get their heads around the fact that you could treat a disease state earlier - it got way confused with Prophylaxis and therefore “No one will pay for it.” If you can’t get people to(especially VCs to understand this) then the funding is doomed.
Let me use the appendix as the example and what we tried to do. We were trying to remove a diseased appendix before it got to the inflamed acute emergency. Because few people understand that the appendix has two phases of acute flare up. One viral (probably) at about the 14 year old mark. The other when you get to about 40 and there are small diverticulum, there are endothelial changes, appendiceal congestion, biomass blockages etc. Often the appendice’s orifice becomes constricted and then you get an acute on chronic even that we all know and love as appendicitis.
We studied this a lot. (Won’t go into it now.)
Our concept was to remove the appendix in the chronic phase of the disease - so during a regular colonoscopy a spyglass could be put into the appendix and you could see the inflammation starting - diverticulum forming - stricture happening - way way before an acute event that would hospitalise people and need emergency surgery. The appendix was diseased - it had pathology that was used in incidental appendectomy to trigger payments. But clinicians could not get off “That’s prophylactic.” NO!!!

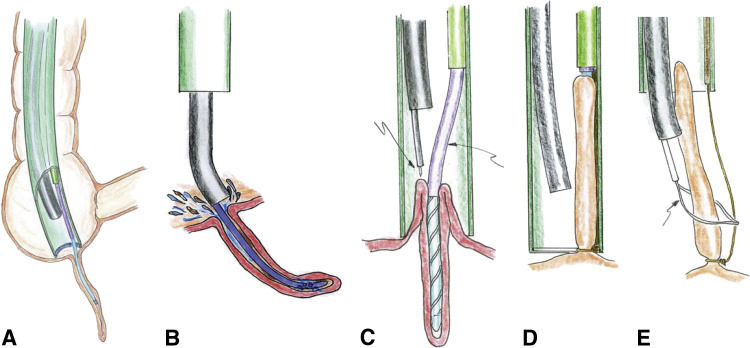
Same with diverticulosis - that is the formation of the small diverticulum. That is a pathological disease state. The acute event is the diverticulitis that brings people in - and ends up with many having a major hemicolectomy. But if the endoscopist had closed off the diverticulae the acute event would never happen and a hemiciolectomy avoided. It was all about less invasive approaches allowing earlier treatment of disease in the chronic phase before an acute attack happened. Way way way too far ahead of its time.
Imagine the economics - if you could eliminate 1/3 of all left hemicolectomies (often with covering Stoma) and multiple reversals ?
But people could not get their heads around it. So it was doomed.
It’s early detection - early “See and treat” - and that is where I will bring us forwards to the future of rendezvous.
Modern thoughts
The issue at the time was there were two schools - the endoscopist and “it has to be treated endoscopically” and the surgeon “It has to be treated surgically.” Both couldn’t get paid right ;) - it’s like the old adage of if you have a hammer - all problems look like nails.
The reality was actually lying right between the two - but people hadn’t fully realised it yet.
In cardiac the cardiologists and the cardiac surgeons had been at war over stents vs CABG. They were also entering the world of endo valve vs open “chest cracking” valve replacement. But there were lots of “Hybrid” procedures performed that actually had amazing results. Indicating the path to the future.
LIMA - LAD via a MIDCAB - and 2 or three stents of the RCA and PDA (Look it up as it’s acronym fantastic and from my cardiac days.) Basically a mixed hybrid cardiac surgery that gives great 20 year results and a cardiology approach - combined to not need to crack the chest.
So in reality these hybrid approaches could avoid cracking the chest - and give superior patient outcomes - and ultimately save money. But people weren’t listening to the data. And many cardiologist preferred to create a “Full metal jacket.” Oh I lament.
But if you can go in and diagnose something, and treat it here and now… brilliant.
So ION and MONARCH are the first two flexible robotic examples I’ll use - and then I’l come onto Endoquest and where we are going. But first let me circle back and help frame the need.

You see what we discovered back in 2007 was that an earlier intervention on a disease state (NOT PROPHYLAXIS… that’s a future post about prophylaxis and preventative medicine I will get into) and using dual modalities could actually start to bring in the concept of precision - early surgery. Or assistive technologies to get higher accuracy. If you could very accurately get to the lesions - identify the lesion and assist from both sides - you start to change the way surgery works.
Now this actually came to my mind by accident and we built on this concept of Rendezvous after seeing a lot of sessile polyps and full thickness resections of sessile polyps. (ESD - Endoscopic Submucosal Dissection) - it is more than just polyps - also mural invasive t=umours etc.
Of then the endoscopic would work from inside the lumen of the gut and tunnel under the sessile (flat) Polyp / Tumour and do a full circumferential resection. Then they would try to be close the defect with different clips and sutures (don’t worry the part about Endoquest is coming.) And sometimes the resection was so deep (it’s thin wall remember) that the endoscopist would end up in the abdomen - and then a lap specialist would be brought in to close the bowel defect.
You got it yet??
So the endoscopist would make the hole from the inside - and the surgeon would close the hole, sometimes stop bleeding from the abdominal side. The two would “Meet up” and hence rendezvous.
One step forward was that some of these cases - they knew ahead of time that it would be a full thickness resection so would set out to meet in the middle.
The challenge from the lumen side was the tools. Flexible manual endoscopes and little ability to suture closed defects. Clips were fine for small defects and would hold the mucosa closed. But not a real defect closure… Also often the scissors were not up to strength - grasping was difficult - and it was all a lot of trial and error for the very few skilled brave interventional endoscopists or colorectal surgeons that also did endoscopy.
But let me come back to this - and in the meantime start to think about going beyond just sessile polyps etc.
See n Treat and beyond
Let me swing on back to ION and MONARCH. These are the robotic bronchoscopes that have been developed by Intuitive and JNJ (well Auris if truth be known) to steer robotically a small bronchoscope to go deeper and further into the terminal bronchioles of the lung - take biopsies and even deliver energy to ablate small tumours (cryo, microwave, electrosurgery.)
Basically the pulmonologist can go to the suspected lesion - biopsy - rapid histology - and ablate if needed - they “See” they “treat” - so see n treat.
Huge cost savings for the health systems - huge anxiety removal for patients - get to tumours earlier and avoid a major surgery.
The alternative can be X ray - CT scan - MRI - see a lesion - send a few weeks later for thoracic surgery and the thoracic surgeon takes out a wedge of lung - or a lobe etc. Taking out more tissue than needed “to be sure.”
Diagnosis - wait - anxiety - major surgery… and two interventions (Hopsital visits) and cost.
And (this is critical) the surgeon is sort of going it “blind.” Yes they have the scans and images - but it is approximate where they will need to resect, so resections are bigger to be sure that all margins are taken. “Less precise” surgery for small lesions.
Okay - what about Rendezvous here? Bingo. Imagine that the ION goes in - finds the lesion - sample - histology and they decide - too big for ablation - and it needs a resection. By good planing if this was done in a hybrid “lab” where imaging and surgery can happen in the same space. The surgeon docks in a daVinci 5 - and the ION talks to the DV5 camera and the exact location of the lesions lights up on the DV5 cockpit display. The surgeon knows exactly - exactly where to resect - they load in a Sureform stapler and do a tiny blebectomy - preserving as much lung as possible. See n Treat (surgical treat) with hyper defined surgical accuracy through two surgical robots guiding each other.
This is where we are going my friends.
It is not the main stream number of DV5 uses - that will still be major surgery - but when a robot company has the endolumenal technology and the transthoracic / abdominal mutiarm robot — we start to get certain cases that make sense.
Hey why stop at multiarm? Hell now the SP really starts too make sense - if we are taking smaller and smaller tissue resections then a single port with a MLC (micro linear cutter) could be all you need to do those small resections.
“Dear robot companies - skate to where the puck is going - you need an endolumenal robot - a single port robot and a multi-arm robot.” - just saying.
Going beyond
We are not going to stop at lung for these rendezvous. Already the urological rendezvous are coming - with the endolumenal robot navigating the urethra - the bladder - the ureters and heading up to the kidney.
From the outside - percutaneous approaches for different renal issues - including stones. Super accurate procedures that are managed from within and externally.
This is already here and now - and is going to accelerate.

But let’s get to the big one and come full circle and start to think about endolumenal gut procedures.
So already we have lots of TAMIS (Trans Anal Minimally Invasive Surgery) happening. It happens in the terminal part of the colon. But with the advent of robots like Endoquest - we can now start to go deeper into the bowel. We can head up past the rectum, the sigmoid - turn the splenic flexure (and when the systems get longer and stronger) we can head to the right colon as well.

From within the colon we will be able to do a lot of the endolumenal procedures like sessile polyps / tumours (ESD) and with the small robotics arms of Endosquest - we can resect with accuracy -and suture close the defects. All though the robotic control. Because these robots have robotic flexible arms that can do complex manoeuvres like suturing with strength.
But we can go one further - we can start to use endolumenal robots to approach known full thickness tumours from the inside. With advanced imaging we will clearly see the tumour boundaries (Cytalux, advanced microscopy and enhanced imaging, new markers.) From inside the colon, or the stomach - we will be able to start a super accurate procedure of resection. We won’t need to take the entire segment of bowel or stomach out. Instead targeted microsurgery where the tumour is removed accurately - and from the outside (let’s say an SP) - blood vessels and blood supply can be managed - adhesions removed - making the endolumenal part faster - safer - easier and above all “doable”.
The two robots meet - and then full thickness surgical closure using suturing from the SP externally and the mucosal closed internally by the endolumenal robot… and now I’m going to give you the kicker….
Who can drive in rendezvous procedures
So back on 2007 / 2008 one of the big barriers was having two specialties need to be in the room at the same time. Because doing complex NOTES / NOS use of the flexible endoscopes was not for the faint hearted.
But step in the robot. And if you look at an Endoquest - it starts to feel very familiar as a control console. Hmm take some of the ION technology - add into the SP instrument technology — and create like and endolumenal SP… and now the surgeon can drive both robots. They know how.
You bring both in - hook to the same DV console - operate the SP for a bit - then click across to the Endo SP - then back - and back and back - and the two robots with one driver can perform the entire rendezvous procedure as a solo surgeon.
The two systems helping each other to navigate with location smarts - mapping systems - where full 3D images can now be created on the fly from both sides. More information - more details - more accuracy all around next generation imaging systems and AI enhanced tumour boundary detection. “Cut here - ablate here - close here.”
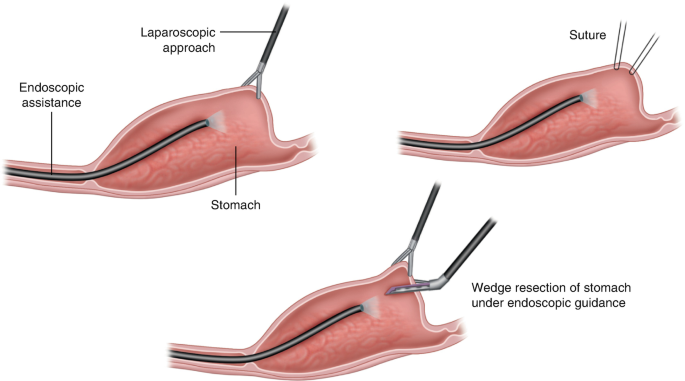
It’s not for every case - but for some of the cases - perhaps the dual robot - rendezvous approach will be the way to get to hyper targeted bowel sparing lesions. New forms of rendezvous bariatric procedures. More aggressive polyp and full thickness tumour removal.
We might start to see the dream I had back in 2006 of treating pathology way earlier before it requires more aggressive surgery.
Cardiac surgeons almost went the way of the dinosaurs because they did not see the cardiologist land grab. I think that general surgeons and thoracic surgeons understand that technology could make them redundant fast - so I think that there is a more open mindset to looking at the endolumenal rendezvous and hybrid approaches. Because it’s coming - and who owns them will determine the future of surgery.
Delivery mechanisms
Let’s think ION and Monarch delivering their highly targeted ablation technologies. And let’s start to imagine that we can do full thickness - hyper targeted resections and then before finishing the surgery from both sides we can deliver ablation - gene therapy - agents with incredible accuracy - in the lung - in the gastric wall - in the bowel. Complimentary therapies delivered at the point of care.
The mix of robots and their cumulative accuracy is going to push diagnosis and see n treat further up the treatment pathway: with minimal microsurgery - accurate approaches - advanced diagnostic realtime cellular level imaging. Delivery of mixed surgery and therapeutic systems of ablation, electric field therapies and drug delivery all at an accuracy never yet seen.
And all of this will start with a single “driver” the interventional surgeon - and as AI and ML improves the accuracy will go up. The rendezvous will get smarter and the micro surgical planning better and better.
The ultimate goal will be earlier diagnosis - treatment - and “tissue sparing” approaches. The advances in technology - accuracy - embedded diagnostics and navigation smarts will drive this faster than people think.
Of course classic surgery will still remain - but if we can take 10% of the patients and give them this less invasive - earlier - tissue sparing type of treatment. The impact on healthcare and patients quality of life will be immense.
2006 I think we were too technologically early - but 2024 and beyond - we are cracking the technology codes, imaging codes, NIR marker codes, ablation energy codes, ML and AI assistance to start to make this a reality.
It is no coincidence that Intuitive created a video about the future (2 years ago) and it is not a coincidence that Intuitive and JNJ have endolumenal robots with ablation technologies, on the market today - along side multi arms (Ottava in development) and Single ports.
It’s not by chance that Medtronic has taken many of the patents of Titan medical. Microport Medbot) “Toumai” has multiarm, single port and endolumenal. In fact they go one further (for another post and have endovacular.
This convergence is going to be a part of the endoscopic arsenal, and it is starting now.
Rendezvous is coming.
These are just speculations and opinions of the author and not reliant upon any inside information. They are predictions based on market trends and historic approaches. It iOS for education purposes only.


